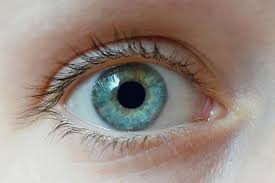
The cornea is a half-sphere-shaped layer that covers the front face of the eye. It is transparent and allows light to pass through it to the pupil and, from there, towards the retina.
Likewise, it protects the iris and lens from external aggressions. It is a powerful refractive lens, allowing approximately two-thirds of the adaptive capacity of the eye to focus. Made up of three different layers separated by two membranes, it is the only organ in the body that lacks blood vessels that supply it, although it is highly innervated, that is, it has a multitude of nerve endings. It is nourished by tears and the aqueous humor of the eye.
How is it produced?
God Service Eye Clinic says that the cornea can suffer different alterations, such as trauma, chronic infections, or shape alterations that reduce its transparency and consequently affect visual capacity. When this happens, on many occasions, the only possible solution is a keratoplasty or corneal transplant.
The cornea bases its refractive capacity on its transparency. If for any reason this is altered, the visual capacity decreases. Below are cases in which transparency may be affected:
- Chronic infections like keratitis, which are typically brought on by bacteria or viruses, can lead to corneal ulcers, resulting in scar tissue that is a little bit duller than the original, healthy cornea.
- Trauma or chemical burns can also make the cornea duller.
- A group of diseases known as corneal dystrophies causes the cornea to become less transparent without triggering an inflammatory response. Both eyes are affected by these changes, which typically start in a person’s early years and advance gradually.
- The normal hemispherical shape of the cornea is changed into a cone in keratoconus, a progressive corneal degeneration, as a result of the central region of the cornea becoming thinner. In most cases, it is bilateral but asymmetrical, and as it worsens, vision becomes increasingly foggy.
- The cornea ages with time, just like all other tissues, and can degenerate in a number of ways. For example, it may develop a peripheral arch (also known as a senile or gerontoxon arch) that has no effect on visual acuity or a scattering of greyish specks that occasionally but not usually impair vision. what is referred to as cornea farinata (floury) affects eyesight.
Symptomatology
The loss of transparency of the cornea will essentially cause a lack of accommodation capacity and consequently, a decrease in visual acuity, being able to see things blurry and distorted. In case of trauma or some infectious corneal lesions, as in the case of herpes, there may also be eye pain, tearing, or purulent discharge.
Diagnosis
The diagnosis will be based on a correct ophthalmological exploration in which the loss of transparency of the cornea, its possible lesions, or alterations in shape will be observed, and its thickness will be assessed.
Treatment
Initially, the lack of transparency of the cornea and its consequent alteration of vision, if they are mild, can be tried to be alleviated with external measures such as glasses or contact lenses. However, if the lesion progresses or causes the patient a lot of discomfort, corneal transplantation must occasionally be resorted to.
Corneal transplantation consists of replacing the damaged cornea with a corneal graft from a cornea donor. The transplant allows for reversing the visual alteration caused by the pathology of the cornea and restoring its normal structure and morphology in case these are altered, as in the case of keratoconus.
Corneal transplantation is performed under local or rarely general anesthesia and is a procedure that usually lasts less than an hour. Using special equipment, the ophthalmologist cuts the part of the cornea that is affected, removes it, and inserts a part of the donor’s cornea of the same size. It is then sutured with a very fine thread that can only be seen at a microscopic level.
In the postoperative period, the eye should be protected, not touched or rubbed, and various antibiotic, anti-inflammatory, and lubricating eye drops should be applied. After the intervention, there may be discomfort. Vision recovery is progressive but slow, it can take months to recover it, but recovery of 90% to 100% of visual capacity prior to corneal involvement is usually achieved. The points are not usually removed in their entirety until after about eight months of the intervention.
Since the cornea has no blood supply, the risk of rejection is very low, with which the success of the transplant is usually assured. The possibility of rejection decreases progressively, being less than 10% after the first year of the intervention. If you feel pain in the transplanted eye, redness, and decreased visual acuity, it may be a rejection, so it is important to contact the ophthalmologist as soon as possible.
Transplant results will vary depending on the underlying corneal pathology. Corneal transplantation gives very good results in keratoconus, for example, or in single lesions, but when there are multiple lesions along the cornea, the results are not so spectacular.
Precautionary measures
For certain pathologies that affect the cornea, such as keratoconus, corneal dystrophies, or degenerations, there are no preventive measures. With regard to infections, care must always be taken to maintain correct eye hygiene and always protect the eyes when exposed to situations in which eye trauma can occur. If corneal opacity appears, it is essential to contact an ophthalmologist as soon as possible.