Physical rehab has always been a combination of skilled clinical evaluation, hands on treatment and therapeutic exercise. The three pillars are central to the effective delivery of rehabilitation. The clinical armamentarium for physical therapists has grown tremendously. Over the last few decades, however, and electricity therapy has taken a special place in the rehabilitation. Field among the many treatments added that have a consistent and well-researched place in rehabilitation. Not to replace the core rehab process, but to serve as a very specific and targeted intervention that targets. Aspects of pain and tissue “dysfunction” that manual therapy and exercise alone can’t reach. And as a result of which are not as efficient as the targeted supplementation intervention.
Electrotherapy is used as part of a comprehensive treatment program at iMotion Physical Therapy. To select and combine the most appropriate modality for each patient’s presentation. Throughout Fremont, San Jose and Los Gatos. That’s why it’s important to know the ins and outs of electrotherapy. The clinical problems it can treat and its place in a comprehensive rehabilitation.
What Electrotherapy Is and How It Works
Electrotherapy is a general term for a group of clinical modalities that employ the application of electrical current. Electromagnetic fields and/or ultrasonic energy to elicit specific therapeutic effects in tissue. The different modalities in this category function in different ways. And treat different clinical issues, so it is important that a knowledgeable physical therapist chooses. The correct electrotherapy device, just as it is important that the device be the proper one.
The most popular electrotherapy modalities in the field of physical rehabilitation. Are transcutaneous electrical nerve stimulation (TENS), neuromuscular electrical stimulation (NMES). Therapeutic ultrasound, and interferential current therapy. They all have their own mechanism, their own clinical indication and their own evidence base to guide their use.
TENS: Pain Management Without Medication
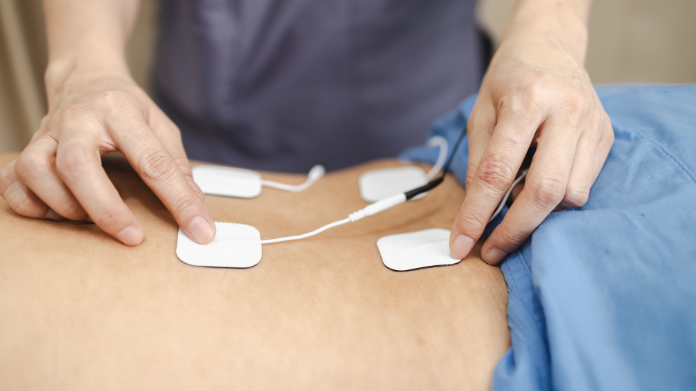
Transcutaneous electrical nerve stimulation involves applying a low-intensity electrical current to the skin. Above and/or near the pain site with surface electrodes. The mechanism is based on the gate control theory of pain: the gate control theory. Pain suggests that stimulation of large diameter sensory nerve. Fibers by the TENS current will inhibit the transmission of pain information. Through the smaller nociceptive fibers into the spinal cord and brain.
The end effect is a decrease in the perceived intensity of pain, without the need for pharmacologic intervention. TENS is a clinically useful tool for pain management for patients in whom therapeutic. Exercise is part of the recovery plan but is limited by pain, such as patients. With post-surgical pain or chronic musculoskeletal pain or acute inflammatory pain.
TENS is incorporated into the treatment plan for back pain. Neck pain, joint conditions and post-surgical rehabilitation. Where it provides patients with the pain reduction. They need to allow them to receive manual therapy and therapeutic exercise at therapeutic dose levels. Which they might not otherwise receive due to pain.
NMES: Restoring Muscle Activation When Exercise Alone Is Insufficient
Neuromuscular electrical stimulation uses a different current protocol from TENS to directly stimulate. Motor nerve fibers, producing muscle contractions in muscles that voluntary effort alone cannot fully activate. This distinction makes NMES one of the most clinically valuable electrotherapy modalities. For a specific and common post-injury and post-surgical problem: arthrogenic muscle inhibition.
Arthrogenic muscle inhibition is the neurological phenomenon in which the sensory response. Of a joint to injury, swelling, or surgical trauma attenuate. The neural drive to the surrounding musculature. The quadriceps after knee surgery, the rotator cuff after shoulder procedures and the deep spinal stabilizers after lumbar injury can all be significantly inhibited in ways that limit the effectiveness of voluntary exercise even when the patient is making maximum effort.
NMES bypasses this inhibition by directly driving motor unit recruitment through the electrical stimulus, producing contractions at levels that voluntary effort cannot achieve in the inhibited state. The muscle is activated, the contraction is performed repeatedly, and the neural pathway for voluntary activation is gradually restored alongside the mechanical conditioning that repeated contraction provides.
At physical therapy Fremont at iMotion, NMES is a standard component of post-surgical rehabilitation protocols for knee replacement, anterior cruciate ligament reconstruction, and shoulder procedures where quadriceps or rotator cuff inhibition would otherwise significantly slow the early rehabilitation timeline.
Therapeutic Ultrasound: Deep Tissue Effects Beyond Vibration
Therapeutic ultrasound uses high-frequency acoustic energy, far beyond the range of human hearing, to produce both thermal and non-thermal effects in deep tissue that surface-applied treatments cannot reach.
The thermal effects of sustained therapeutic ultrasound application increase the temperature of deep connective tissue, tendon, and muscle, improving collagen extensibility and enhancing the viscoelastic properties of the tissue in ways that make subsequent manual therapy and stretching more effective. This pre-treatment application is particularly valuable for tight, fibrotic tissue around healing surgical sites, chronic tendon conditions, and joint capsule restrictions that limit range of motion.
The non-thermal effects of pulsed therapeutic ultrasound, produced through the acoustic streaming and cavitation that the oscillating pressure waves generate in tissue fluid, influence cellular membrane permeability and stimulate tissue repair processes at a biological level. These effects have been studied most extensively in the context of soft tissue healing, tendon repair, and the management of chronic wound healing — areas where the stimulation of biological repair activity provides a meaningful clinical addition to conventional rehabilitation.
Conclusion
At physical therapy San Jose California at iMotion, the full range of electrotherapy modalities is available alongside the aquatic therapy capabilities of the Motion Plus Aquatic and Therapy Center, creating a comprehensive rehabilitation environment where electrotherapy is integrated within treatment plans built around each patient’s complete clinical picture.
Interferential current therapy, which uses the intersection of two medium-frequency electrical currents to produce a low-frequency therapeutic effect in deep tissue with minimal patient discomfort, provides an additional pain management and tissue stimulation option for patients where TENS or ultrasound alone is insufficient.
Laser therapy, available at iMotion San Jose and Fremont, uses specific wavelengths of light to support cellular energy production, reduce tissue inflammation, and accelerate the healing response in injured and post-surgical tissue. While not a traditional electrotherapy modality in the strict sense, it shares the characteristic of providing a targeted biological stimulus that exercise and manual therapy cannot deliver — and it is often combined with electrotherapy modalities within the same treatment plan for a cumulative effect.
The principle that guides electrotherapy use at iMotion across all locations is clinical specificity: selecting the modality whose mechanism best addresses the specific tissue dysfunction present in each patient’s case, at the appropriate stage of their recovery, in combination with the manual and exercise-based treatment components that drive the overall rehabilitation outcome.
Electrotherapy does not replace clinical expertise. In the hands of skilled therapists at Physical Therapy Fremont and Physical Therapy San Jose California, at iMotion, it extends what that expertise can achieve.